Category: Opioid
-

2023 Prescribing and Pharmacology of Controlled Drugs Conference
The Medical Association of Alabama hosted its annual meeting on November 18-19, 2023, at the Hyatt Regency Birmingham-The Wynfrey Hotel in Birmingham, Alabama. The focal point of this gathering was the renowned “Prescribing and Pharmacology of Controlled Drugs Conference,” marking the 15th year of its occurrence and the 45th presentation of the 12-hour Prescribing and…
-

The 11th Circuit Applies SCOTUS Ruling In Recent Alabama Physician Controlled Substances Conviction
By: Jim Hoover with Burr & Forman, LLP On June 27, 2022, the Supreme Court of the United States (SCOTUS) heard an appeal emanating from a conviction of a local doctor in Mobile, Alabama for violating the Controlled Substances Act (CSA). The justices specifically examined the convictions of Dr. Xiulu Ruan who is serving a…
-
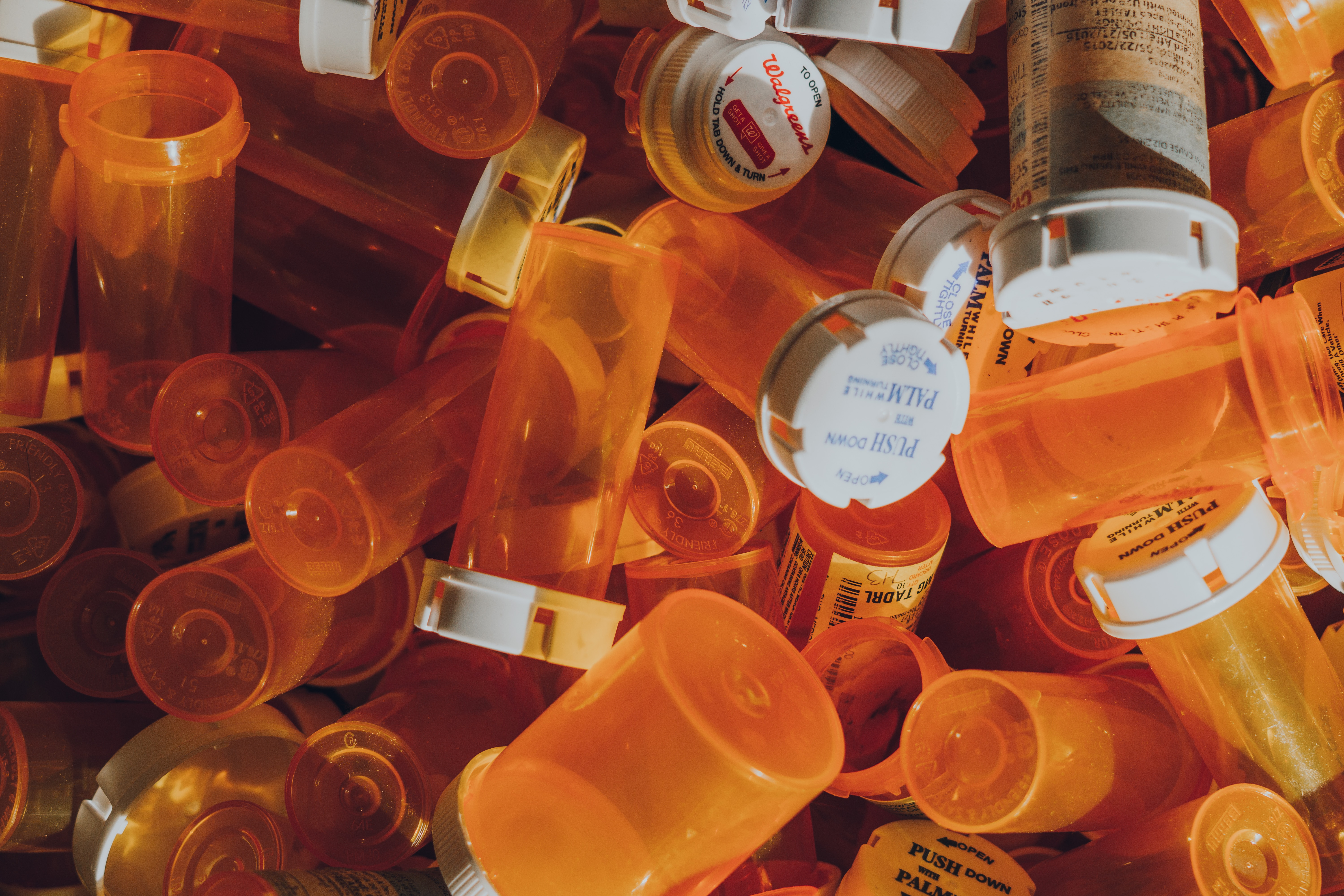
Opioid Prescriptions in Alabama Fall for 8th Consecutive Year
Contact: Jeff Emerson, 205-540-2247MONTGOMERY – Alabama physicians are taking action to reduce the number andpotency of opioid prescriptions and to increase access to medication that rapidlyreverses opioid overdoses, according to a new report released Thursday from theAmerican Medical Association. The report shows:• Opioid prescriptions in Alabama decreased 41.6 percent from 2012-2021. From2020-2021, opioid prescriptions in…
-
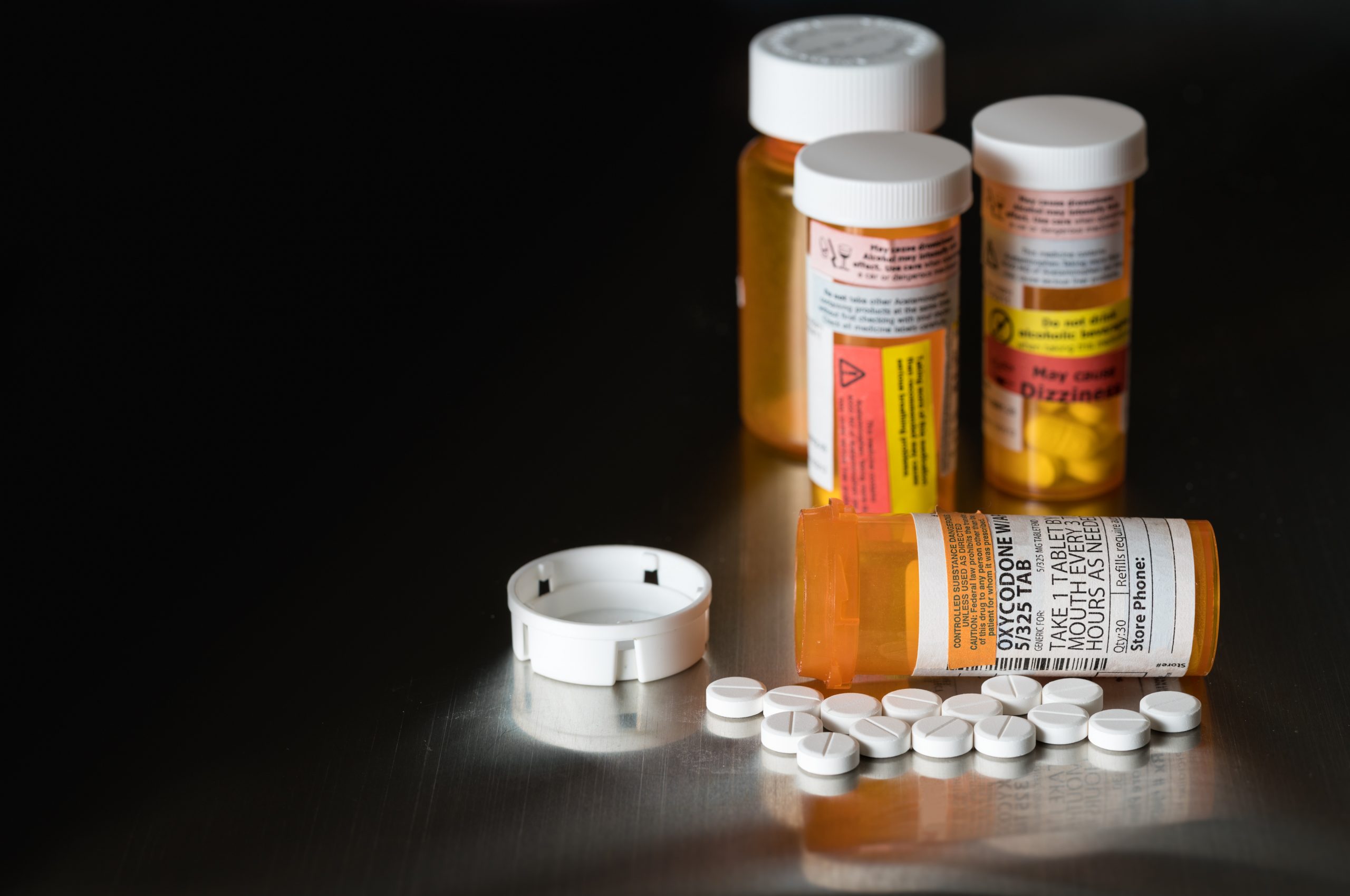
America’s ‘Other’ Health Emergency Needs Attention Too
Drug overdose deaths could surpass 100,000 in the U.S. for the first time ever By John Meigs, Jr., MD For the past 12 months, the nation’s medical community correctly and understandably focused nearly all its attention on the COVID-19 pandemic. Now with millions being vaccinated, we are hopefully about to turn the corner and can…
-

Report: 34 Percent Decline in Opioid Prescribing since 2014
FOR IMMEDIATE RELEASE CONTACT: Mark Jackson, Executive Director (334) 954-2500 CONTACT: Mallory Camerio, Director of Communications (334) 954-2580 Report: 34 Percent Decline in Opioid Prescribing since 2014 According to a new report released by the American Medical Association, Alabama physicians have reduced opioid prescribing by 34.4% since 2014, increased the use of state prescription drug…
-

Alabama Hospitals File Suit Against Opioid Manufacturers, Distributors
Hospitals experience significant financial and operational harm as opioid crisis continues EVERGREEN, Ala., Sept. 10, 2019 /PRNewswire/ — After two decades of providing frontline care in response to the opioid crisis, a group of 21 Alabama hospitals have filed a civil lawsuit in Conecuh County Circuit Court against the manufacturers, distributors, and retailers of opioid-based drugs.…
-
Opioid Use Decreased in Medicare Part D While MAT Increased
The nation has been grappling with an opioid crisis for years. In 2017 alone, there were 47,600 opioid-related overdose deaths in the United States. It continues to be a public health emergency. U.S. Department of Health & Human Services Office of the Inspector General has been tracking opioid use in Medicare during this crisis, particularly…
-
CDC Clarifies Opioid Prescribing Guidelines
Since the Centers for Disease Control and Prevention released its Guidelines for Prescribing Opioids for Chronic Pain in 2016, physicians have relied on the document for recommendations when prescribing pain medication to their patients. However, because the CDC did not specifically clarify the guidelines in the original release, many physicians’ groups have been concerned the…
-

Drug Overdoses in Young People on the Rise
PISCATAWAY, NJ – In American adolescents and young adults, death rates from drug poisoning, particularly from opioids, have sharply increased over the last 10 years, according to new research in the Journal of Studies on Alcohol and Drugs. In 2006, the death rate from drug poisoning from any type of legal or illicit drug was 8.1…
-

New Statistics Show Doctors Positively Impacting Opioid Epidemic
MONTGOMERY — Alabama’s physicians are having a positive impact on the opioid epidemic here at home while national statistics are showing for the first time, Americans’ odds of dying from an accidental opioid overdose are higher – 1 in 96 – than from a motor vehicle crash – 1 in 103. Using data from the…