Tag: Blue Cross
-
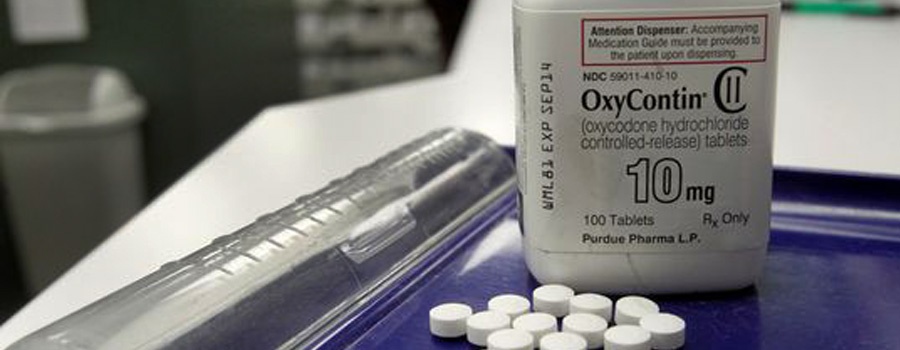
BCBS Alabama to No Longer Cover OxyContin Beginning in 2019
BIRMINGHAM, AL – Effective Jan. 1, 2019, Blue Cross Blue Shield of Alabama will no longer cover OxyContin for members with the exception of Blue Advantage members. This is in response to concerns for members’ care and safety. Since 2015, opioid prescriptions in the U.S. and in Alabama have declined. Over the last two years,…
-

CVS Out of BCBS Alabama Network but Does Not Affect PIPA Policies
While some Blue Cross and Blue Shield customers in Alabama will no longer be able to use CVS for their prescription drugs, the Medical Association members who have PIPA policies will not be affected. CVS is no longer in the Blue Cross and Blue Shield Alabama preferred network for certain plans, and according to the…