Tag: morphine
-
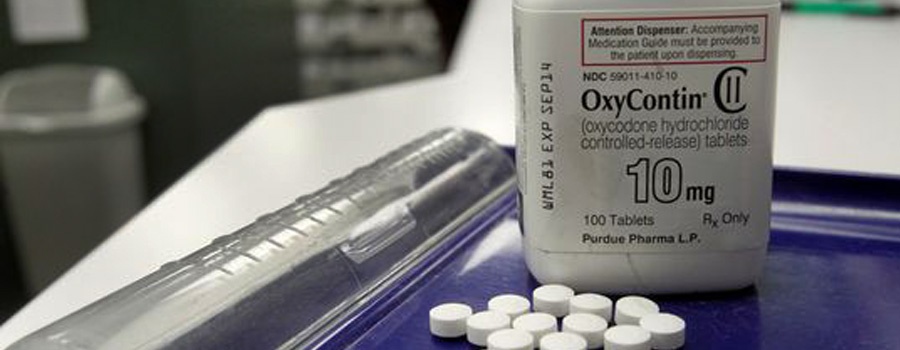
MME Edit Coming in Early 2019
The Alabama Medicaid Agency is working on implementing Morphine Milligram Equivalent (MME) edits in early 2019. Higher doses of opioids are associated with higher risk of overdose and death – even relatively low dosages (20-50 MME per day) may increase risk. Therefore, beginning in early 2019, Alabama Medicaid will limit the amount of cumulative MME’s allowed per…
-

Just What the Doctor Ordered: An Alabama Perspective on the Opioid Epidemic
Sometimes, Alabama is No. 1. In 2012, Alabama was the highest per capita painkiller prescribing state, with an average of 143 prescriptions written per 100 people — almost three times the rate of the lowest prescribing state.1 Alabama has been home to other No. 1s, too. In 2012, Dr. Shelinder Aggarwal, a former Huntsville-area pain…